 All patients in all 18 studies were clinical axillary node negative. 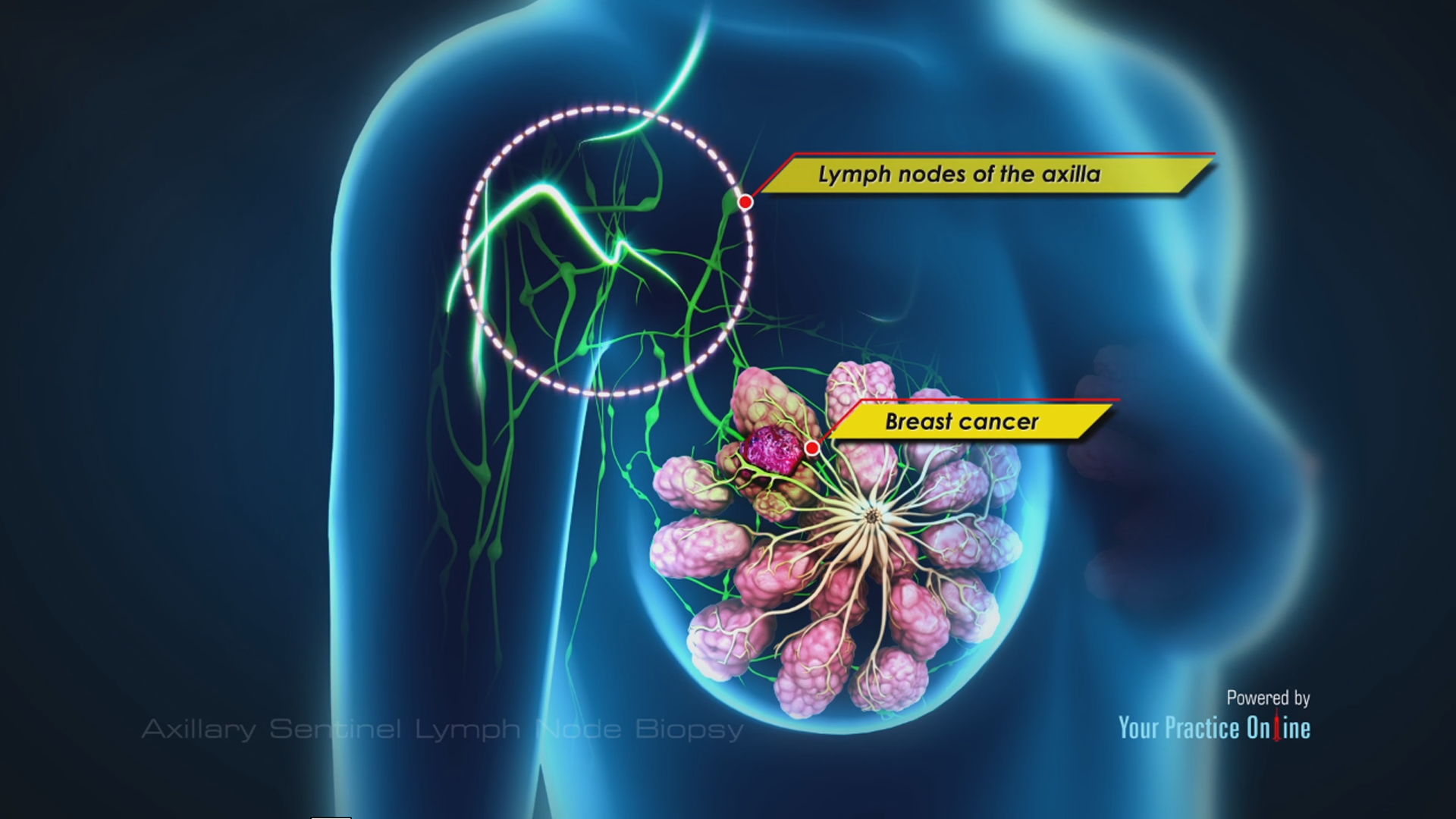
All of the studies included a group of patients for which MBD alone was used as the mapping technique for SNB. Five studies were from China, 2 were from Turkey, and 1 study each was from Chinese Taipei, Egypt, Italy, the United States, the United Kingdom, Jamaica, Greece, India, Serbia, Pakistan, and Indonesia. The 18 studies were published between 20. Our search strategy is presented in Fig 1. Two-sided P-values < 0.05 were considered significant.Ī total of 1,559 patients in 18 studies that met the inclusion criteria were analyzed in our meta-analysis. The effect of MBD dose and injection site on the IR and FNR was determined using the chi-squared test. Publication bias was displayed graphically using funnel plots. For outcome measures without significant heterogeneity among studies (P > 0.10), proportions were calculated using a fixed-effect model otherwise, a random-effect model was employed. The heterogeneity of the studies was evaluated using the inconsistency statistic (I 2). Individual studies were weighted by study size and by the inverse of the variance of individual point estimates. The meta-analysis of IR, FNR, accuracy rate (AR), negative predictive rate (NPV) and SNB sensitivity was conducted using the metaprop function in the R-meta package. Four test performance parameters were evaluated: sensitivity, FNR, NPV, and AR. The results of each successfully identified SN were further categorized as true positive (TP), true negative (TN), or false negative (FN). The IR for SNB was defined as the number of patients with successfully identified SNs divided by the total number of patients for whom SNB was attempted. The meta-analysis in this study was conducted using R version 3.2.2 for Windows (R: A language and environment for statistical computing R Foundation for Statistical Computing, Vienna, Austria, ). Thus, we performed the present meta-analysis to collect data to assess the feasibility and accuracy of SNB mapped with MBD alone in patients with breast cancer. Although several studies have used MBD alone to map SNs in breast cancer, the patient selection criteria and details of the mapping methods varied across individual studies. Thus, the use of MBD alone as a mapping method for SNB seems feasible and may expand the use of SNB in developing countries. Recently, several studies reported that blue dye alone was sufficient for identifying SNs in breast cancer. Simon first reported that MBD could serve as an alternative to isosulfan blue in combination with radioisotopes for SNB in breast cancer, and similar conclusions were drawn by other researchers. MBD is cheaper than patent blue or isosulfan blue and is easier to obtain in developing countries. Therefore, MBD alone is sometimes used to map SN localization in these countries. Furthermore, in these countries, there is limited access to patent blue and isosulfan blue. Concern about the hazards of radiation exposure is also an obstacle for the use of the combined method. Although the radiation exposure during SNB using radioisotopes is limited and is safe for pregnant surgeons and patients. 
Unfortunately, many hospitals in developing countries, including China, do not currently have the ability or qualifications to provide nuclear medicine and equipment. Although there is no standard mapping technique for SNB, the combination of blue dye and radioisotope techniques is thought to be more reliable and is currently the most widely used method for SNB mapping in breast cancer. Several studies have reported that the combined use of blue dye and radioisotopes is significantly superior to blue dye alone for SNs identification. 
Krag investigated the use of radioisotopes for SN identification, while Albertini was the first to identify the SN using a combination of blue dye and radioisotope techniques. Giuliano conducted intraoperative lymphatic mapping and identified the SN using only blue dye. The mapping method is one of the most important factors affecting the identification rate (IR) and false negative rate (FNR) of SNB in breast cancer. 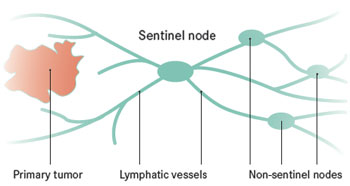
As a minimally invasive surgery, SNB can accurately stage the axilla and leads to less morbidity than axillary lymph node dissection (ALND). Currently, SNB has become a standard procedure for axillary staging in early breast cancer. The sentinel lymph node (SN) concept was soon adopted for use in breast cancer patients and led to significant improvement in the management of the axilla in breast cancer surgery. Sentinel lymph node biopsy (SNB) was first reported in cutaneous melanoma by Morton et al. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
